Patient stories
Improving treatment for infants with epilepsy
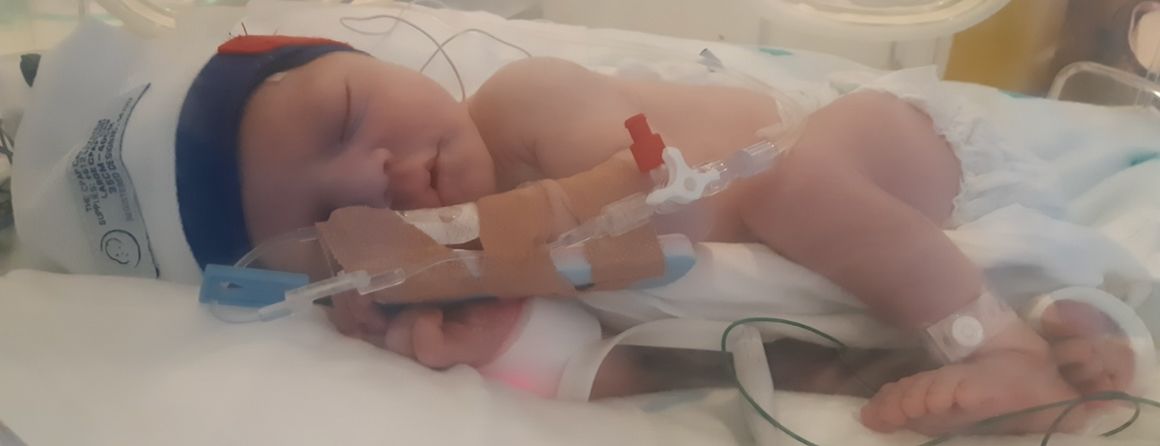
Levi Trowbridge was just three days old and newly released from the maternity ward when he went into convulsions.
Within a week, Levi was transferred to The Royal Children's Hospital in Melbourne and put under the care of Dr Katherine Howell, the epilepsy team leader at Murdoch Children's Research Institute and a pediatric neurologist at The Royal Children's Hospital.
Although Levi's initial diagnosis was early infantile epileptic encephalopathy, he had other worrisome symptoms, in addition to his frequent seizures.
"He was floppy and lethargic and, for a time, needed support with his breathing and feeding," said Dr Howell, who subsequently arranged for Levi to take part in a rapid genomic testing program for critically ill children at the Victorian Clinical Genetics Services, the genetic testing arm of MCRI.
Levi was diagnosed with KCNQ2 epileptic encephalopathy, a rare genetic disorder that causes frequent seizures.
"Levi was three days old and I had just brought him home from the hospital when he had his first major seizure," said Karsha, Levi's mum. "It was a terrifying time, watching your baby having multiple seizures a day, and at times, turning blue and holding his breath. Levi was on life support when he was at his weakest and there were days when we weren't allowed to hold him because it could affect his test results. But when we got a diagnosis that changed everything. We were no longer kept in the dark, not knowing how to help our child."
Ms Trowbridge said after changing medications Levi went from having five seizures a day to not having any since February 2020.
"Levi improved rapidly and his multiple daily seizures stopped by the time he was three weeks old, he was more alert, started to feed well and was able to go home from the hospital," said Dr Howell.

Medical experts around the world hope to learn from infants with epilepsies experiences to improve treatment for infants with epilepsy through The International Precision Child Health Partnership, or IPCHiP.
The project has brought together four major pediatric centres – the Murdoch Children's Research Institute with The Royal Children's Hospital and the University of Melbourne; The Hospital for Sick Children (Toronto, Canada); Boston Children's Hospital (Boston, USA) and the UCL Great Ormond Street Institute for Child Health and Great Ormond Street Hospital (London, UK) – to pool together their medical and scientific expertise to analyse medical and genomic data to accelerate discovery and therapeutic development.
"Having a prompt genetic diagnosis guided our choice of seizure medication, with dramatic effect. Most other antiseizure medications wouldn't have worked for Levi. We've had a glimpse with individual babies like Levi of the possible benefits of prompt genetic diagnosis, but we now want to understand how much benefit this approach might provide to all the infants we see with these devastating conditions," Dr Howell said.
"In Melbourne, we only see about 30 babies like Levi every year, but by following the outcomes of hundreds of infants with epilepsy who receive cutting-edge genetic sequencing, genetic counselling and precision treatments across the IPCHiP consortium, we will be able to treat genetic epilepsy faster, more precisely and with better outcomes."

