Written by Dr Monica Cooper | Honorary Research Fellow, Developmental Disability and Rehabilitation Research, Clinical Sciences, Murdoch Children's Research Institute and Dr Mark Mackay | Director of the Children's Stroke Program, Neuroscience Research, Clinical Sciences, Murdoch Children's Research Institute.
Children with cerebral palsy are more likely to develop seizures – but it's not all bad.
Our recent study, Seizures in Children With Cerebral Palsy and White Matter Injury (2017), found that children with cerebral palsy generally have seizure types that are exactly the same as children that don't have cerebral palsy and are developing normally.

These particular seizures occur infrequently and respond well to medicine. This discovery gives us the ability to provide reassurance to parents that medication usually works well when it comes to treating seizures. There is also a good chance their children will outgrow their seizures as they move into their teens!
Not only does this help to reassure parents, but clinicians often presume that if a child has cerebral palsy, they will most likely have seizures that will be difficult to control.
Paediatricians are also used to treating kids with these types of seizures – so this finding gives doctors a better understanding of how to treat patients with cerebral palsy who have seizures.
Cerebral palsy is an 'umbrella term', making this a very mixed group of children to study. There are multiple causes of cerebral palsy, which include prematurity, stroke, infection, hypoxia and genetic causes. Given the many causes of cerebral palsy, it is important to ensure that the causes of cerebral palsy are carefully separated when conducting research.
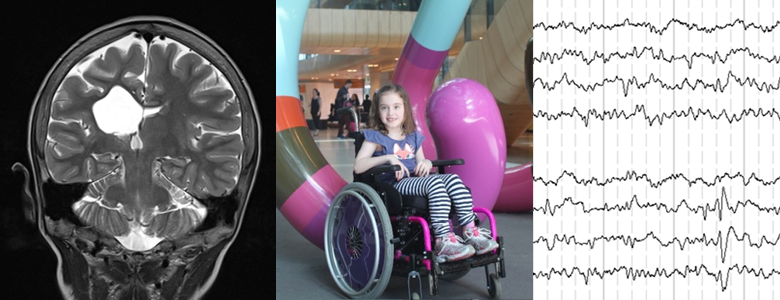
White matter injury is the most common type of injury seen in people with cerebral palsy, which is most likely due to a bleed, stroke or not enough blood flow to the brain. As part of the study, we carefully reviewed MRI scans of children born with cerebral palsy and white matter abnormalities. If the pattern on the MRI was not consistent with this injury, children were excluded.
Currently, the epilepsy classification for these epilepsy syndromes does not allow for children with brain injury or malformations – but perhaps it's time that it did. Our research identified that one in five children with cerebral palsy and white matter injury will have seizures that fit with a recognised childhood epilepsy syndrome.
Dr Simon Harvey, co-author and Director of the Children's Epilepsy program said "Just because a child has a brain injury, it does not mean that their seizures will be lifelong, or that they are directly related to that injury."
These discoveries can also be used for research into other developmental disabilities.
Seizures can be very frightening for families, which is why this research is so important. We would like to thank the patients and their families for their participation. We could not have completed this work without their help and time.
Lead researcher, Dr Monica Cooper is a General Paediatrician working in the Department of Neurodevelopment & Disability. She is also a PhD candidate in the Department of Paediatrics, The University of Melbourne and an Honorary Research Fellow at Murdoch Children's. She has presented her PhD findings at national and international conferences.



