A weighty matter: exploring body mass index in Duchenne muscular dystrophy
Zoë Davidson PhD, Accredited Practising Dietitian
Overweight and obesity is a problem facing all Australians including our own children. Currently, one in four Australian children are overweight or obese; a scary statistic. But what if I was to tell you there are a group of children in which one in two are obese? Would you believe me? This is the alarming truth facing boys with Duchenne muscular dystrophy (DMD).
DMD is a neuromuscular disease that causes progressive and relentless muscle weakness in boys, leading to loss of the ability to walk around the early adolescent years. Recently, there have been considerable developments in treatment, specifically the use of certain hormones (steroids, but not the ‘bodybuilder’ type) to maintain strength and function. Yet despite these advances, the nutritional issues associated with DMD are complex and poorly understood.
Current nutritional recommendations are based almost solely on two research papers published in the 1990s in patient cohorts not treated with hormones. There was an obvious need for this research to be updated, not only in the context of steroid treatment, but also using standardised assessments. Hence, the aim of this study, led by researchers within the Murdoch Children's Research Institute Centre of Research Excellence in Neuromuscular Disorders, was to describe body mass index (BMI) patterns in a cohort of boys with DMD using steroids.
Weight is usually defined by body mass index (BMI): the relative weight based on an individual's mass and height. Adults with a BMI between 20 and 25 are considered to have a healthy weight, those between 25 and 25 are classed as ‘overweight’ and those over 30 as ‘obese’. Assessment of BMI in children and teens is based on growth charts.
Our retrospective cohort (a group of individuals studied over time) measured BMI over time in 144 boys with Duchenne seen in two Australian clinics, 72% of whom were currently or had previously used steroids.
As the graph demonstrates, we found that obesity is prevalent across all ages, reaching almost 50% in 10 year olds. This is shockingly high when compared to population data in which the prevalence of obesity ranges from 4-7%. Although not shown on this graph, the prevalence of underweight boys with DMD increased steadily from about 10 years of age. 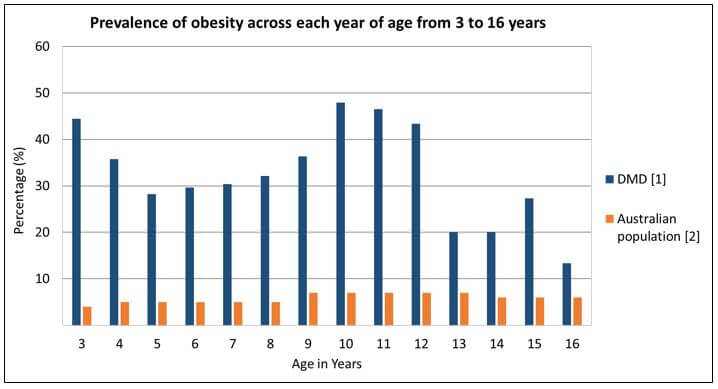 [1] Davidson et al. Eur J Clin Nutr. 2014 Aug;68(8):892-7.
[1] Davidson et al. Eur J Clin Nutr. 2014 Aug;68(8):892-7.
[2] 2007 Australian National Children’s Nutrition and Physical Activity Survey
So does obesity matter in DMD?
Whilst in the Neuromuscular clinic we see the significant impact that increased weight has on a patient’s walking and strength, there is only anecdotal evidence to support this. In fact, we know very little about the relationship between weight status and clinical outcomes.
So what are we doing about this?
Within the Neuromuscular clinic at the Royal Children’s Hospital, we have introduced clinical protocols whereby all boys with DMD will see a dietitian annually. In addition, their growth will be reviewed by a dietitian at every clinic visit.
We are also embarking on crucial research to understand the relationship between growth, function, and energy expenditure. This funded study will inform a much-needed and long-awaited weight management intervention for DMD.
Ultimately, we hope these investigations will make life just a little easier for boys who are obviously struggling with their weight on top of living with this devastating condition.
For more information about research in neuromuscular disorders at Murdoch Children's Research Institute visit the Centre of Research Excellence in Neuromuscular Disorders.
The Murdoch Children's Research Institute may publish material submitted to the blog at its sole discretion. The Institute accepts no liability in respect of any material published or the content and accuracy of any material published. If you have any concerns with any of the published material or comments on the blog, please contact us at show email address



