Understanding how newborns' brains respond to anaesthesia

For babies born extremely premature, like twins Mikey and Gabe, the fight for life starts from the first breath. They have great odds of survival, but if surgery is required and an inadequate anaesthesia dose is administered, their quality of life can be severely impacted.
At 25 weeks old, a baby's brain is busy processing what they see and hear. The baby's brain, lungs and digestive system are formed but not fully developed.
These babies have around an 80 per cent chance of surviving, but they need help in intensive care to breathe for some time. Surgery is sometimes needed too, which requires delicate newborn anaesthetic care.
With inadequate anaesthesia, babies mount a profound stress response to surgery that can lead to brain injury. Untreated pain has long-term effects, including behavioural changes and altered pain sensitivity that may persist for decades. Excess anaesthesia may lead to post-operative breathing problems, low blood pressure or toxicity.
To help better understand the effect of anaesthetics on neonatal brains, Murdoch Children's Research Institute (MCRI) PhD student and The Royal Children's Hospital anaesthetist Dr Sebastian Corlette and his team are measuring newborn's brainwaves during surgery using electroencephalogram (EEG), a test that detects electrical activity in the brain using small, metal sensors called electrodes attached to the scalp.
Brain cells communicate via electrical impulses and are active all the time, even when you are asleep or under anaesthesia. This activity shows wavy lines on an EEG recording, which Dr Corlette uses to measure how newborns' brains behave while anaesthetised.
"The newborn brain is different to the adult brain. It is small, functionally immature, and rapidly growing," Dr Corlette said. The vast developmental changes, along with the immaturity of body systems, make the actions of drugs highly variable in these patients. Too little or too much anaesthesia each pose a risk of harm to newborns."
Dr Corlette said there was a wide variation in practice when anaesthetising newborns, however, there were few studies that measured anaesthetics in this highly vulnerable group.
"It's early days for our research, but we already have some very interesting results," he said.
"Newborns show larger and longer-lasting changes in their EEG than older patients do, and with very low doses of anaesthesia. These changes differ from EEG patterns that we see naturally in the developing brain and they vary with different anaesthetic doses."
Dr Corlette said he hoped that anaesthetists would better understand how newborns' brains respond to anaesthesia through this research, and he aimed to create a method to formally evaluate different strategies.
"In the future, we want to develop controlled clinical trials to evaluate different anaesthesia regimens and answer some of the large gaps in our knowledge about neonatal anaesthesia," he said.
Seeing the benefits of newborn anaesthesia, Sean and Emily Leyden enrolled their son Mikey in Dr Corlette's study.
"The first six weeks of the boys' lives were a nightmare rollercoaster," Sean said. "It was literally life or death. They needed ongoing care for the first three months of their lives."
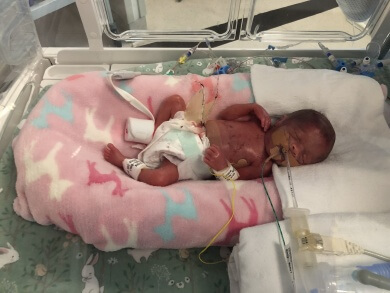
Gabe, fortunately, did not have any complications. However, on day four of the twins' lives, a hole formed in Mikey's (pictured, left) small intestine. He was rushed from the Royal Women's Hospital to The Royal Children's Hospital (RCH) for immediate surgery.
Paediatric surgeon Dr Tom Clarnette operated on Mikey while Dr Corlette administered the anaesthesia. Due to his condition, Mikey stayed at The RCH, while Gabe remained at the Royal Women's.
"For three months, we spent a minimum of four hours a day in each hospital with each boy, and we didn't know what would happen from day to day," Sean said. Once we got through that first six weeks, things settled down to more of a week-to-week situation, and it became more sustainable, but it's been a very difficult journey overall."

After three months, Gabe was released from the hospital, and Mikey could finally join him two weeks later.
"We reunited them as soon as we could, and they were definitely happy to see each other, Sean said. "It's a dream come true to have them home finally. That's what we've been working towards for three months, so it's just fantastic."
Sean and Emily have enrolled the twins in three more studies and hope that other babies can benefit from medical research too.
"If the trials are non-invasive, ethical, and involving research, we want to support them," he said.
Funding:
This project is supported by a SPANZA Research Grant, ANZCA Emerging Researcher Scholarship, Melbourne Children's Postgraduate Health Research Scholarship and funding from the Australian Society of Anaesthetists.
At 25 weeks old, a baby's brain is busy processing what they see and hear. The baby's brain, lungs and digestive system are formed but not fully developed.
These babies have around an 80 per cent chance of surviving, but they need help in intensive care to breathe for some time. Surgery is sometimes needed too, which requires delicate newborn anaesthetic care.
With inadequate anaesthesia, babies mount a profound stress response to surgery that can lead to brain injury. Untreated pain has long-term effects, including behavioural changes and altered pain sensitivity that may persist for decades. Excess anaesthesia may lead to post-operative breathing problems, low blood pressure or toxicity.
To help better understand the effect of anaesthetics on neonatal brains, Murdoch Children's Research Institute (MCRI) PhD student and The Royal Children's Hospital anaesthetist Dr Sebastian Corlette and his team are measuring newborn's brainwaves during surgery using electroencephalogram (EEG), a test that detects electrical activity in the brain using small, metal sensors called electrodes attached to the scalp.
Brain cells communicate via electrical impulses and are active all the time, even when you are asleep or under anaesthesia. This activity shows wavy lines on an EEG recording, which Dr Corlette uses to measure how newborns' brains behave while anaesthetised.
"The newborn brain is different to the adult brain. It is small, functionally immature, and rapidly growing," Dr Corlette said. The vast developmental changes, along with the immaturity of body systems, make the actions of drugs highly variable in these patients. Too little or too much anaesthesia each pose a risk of harm to newborns."
Dr Corlette said there was a wide variation in practice when anaesthetising newborns, however, there were few studies that measured anaesthetics in this highly vulnerable group.
"It's early days for our research, but we already have some very interesting results," he said.
"Newborns show larger and longer-lasting changes in their EEG than older patients do, and with very low doses of anaesthesia. These changes differ from EEG patterns that we see naturally in the developing brain and they vary with different anaesthetic doses."
Dr Corlette said he hoped that anaesthetists would better understand how newborns' brains respond to anaesthesia through this research, and he aimed to create a method to formally evaluate different strategies.
"In the future, we want to develop controlled clinical trials to evaluate different anaesthesia regimens and answer some of the large gaps in our knowledge about neonatal anaesthesia," he said.
Seeing the benefits of newborn anaesthesia, Sean and Emily Leyden enrolled their son Mikey in Dr Corlette's study.

"The first six weeks of the boys' lives were a nightmare rollercoaster," Sean said. "It was literally life or death. They needed ongoing care for the first three months of their lives."
Gabe, fortunately, did not have any complications. However, on day four of the twins' lives, a hole formed in Mikey's (pictured, left) small intestine. He was rushed from the Royal Women's Hospital to The Royal Children's Hospital (RCH) for immediate surgery.
Paediatric surgeon Dr Tom Clarnette operated on Mikey while Dr Corlette administered the anaesthesia. Due to his condition, Mikey stayed at The RCH, while Gabe remained at the Royal Women's.
"For three months, we spent a minimum of four hours a day in each hospital with each boy, and we didn't know what would happen from day to day," Sean said. Once we got through that first six weeks, things settled down to more of a week-to-week situation, and it became more sustainable, but it's been a very difficult journey overall."

After three months, Gabe was released from the hospital, and Mikey could finally join him two weeks later.
"We reunited them as soon as we could, and they were definitely happy to see each other, Sean said. "It's a dream come true to have them home finally. That's what we've been working towards for three months, so it's just fantastic."
Sean and Emily have enrolled the twins in three more studies and hope that other babies can benefit from medical research too.
"If the trials are non-invasive, ethical, and involving research, we want to support them," he said.
Funding:
This project is supported by a SPANZA Research Grant, ANZCA Emerging Researcher Scholarship, Melbourne Children's Postgraduate Health Research Scholarship and funding from the Australian Society of Anaesthetists.



