Kidney Regeneration
Our vision is to develop new treatments for inherited and chronic kidney disease. Using human stem cells to recreate kidney tissue, we hope to model kidney disease, find new therapies, and eventually develop replacement organs.
The kidney is a complex and essential organ required for maintaining fluid balance, blood volume, and electrolyte stability in the body.
The kidneys are essential organs that maintain fluid balance, blood volume, and electrolyte balance. In humans, all these functions are achieved by the approximately 1,000,000 individual nephrons present in each adult kidney. Remarkably, all of these nephrons are formed before birth, hence any disease no new nephrons can form.
In our research group, we have used our understanding of how the nephrons form during normal kidney development to recreate a model of the human kidney using pluripotent stem cells. These stem cell-derived mini-kidneys can be made using cells from patients with kidney disease.
They can also be generated using gene-edited stem cells engineered to recreate a disease state or a readout of function. Using stem cell-derived models of inherited kidney disease, we aim to screen for novel treatments. We also aim to engineer human kidney tissue to provide a source of renal replacement other than dialysis and organ transplantation.
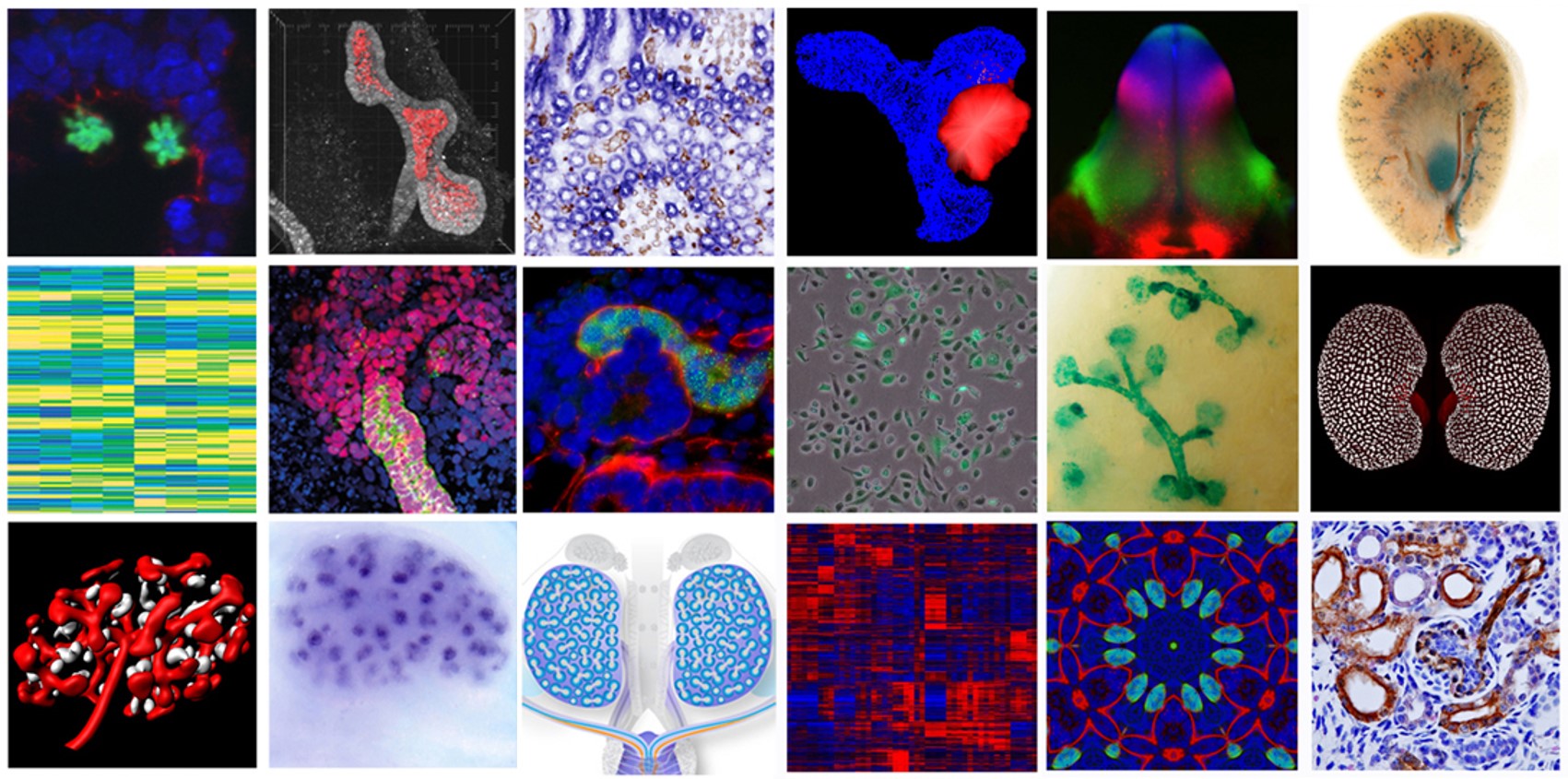
Understanding, improving, and applying human pluripotent stem cell-derived kidney tissues
MCRI researcher, Professor Melissa Little spoke with Joel Topf, MD at American Society of Nephrology (ASN) Kidney Week 2024 about her research.
Group Leaders

Team Leaders


Group Members













Our projects
Rebuilding the kidney using human pluripotent stem cells
The prevalence of chronic kidney disease is continuing to rise worldwide, and with limited treatment options available and a shortage of suitable donor organs, there is a genuine need for new treatment options.
Our laboratory has pioneered methods of using stem cells to grow mini kidneys, also known as kidney organoids in the lab. Ultimately, the utility of these mini-kidney tissues will depend on how effectively they mature and replicate a normal kidney and we are currently working toward improving the structure, size and function of these organoids.
Further understanding the genetic pathways involved in the formation and maturation of each cell type during kidney development will help us better replicate normal development in a dish.
We expect this research to be revolutionary to kidney disease treatment options via two avenues: one is through patient-derived disease modelling and drug screening approaches that further our understanding of kidney diseases and lead us toward new treatment options; the second is through the regeneration of kidney tissue for transplant or the development of artificial kidneys,
Modelling kidney disease in a dish using patient-derived stem cells and drug screening
One key area of our kidney research focuses on creating stem cells from patients and recreating their kidney tissue or mini kidney organoids in our laboratories. This allows us to recreate and study their disease more closely–this method of research is called disease modelling.
If we can determine a genetic cause for the disease by studying a patient’s tissue in the laboratory, we now have the gene-editing capability and technology to correct mutations found in that patient’s genome. By comparing a patient’s genetically mutated and corrected cell lines, we can better understand a disease’s cause and progression, which informs our understanding of any potential preventative measures, tests for that disease, development of new treatments and hopefully cures.
We are also investigating whether mini-kidneys can screen for drugs that cause damage to kidney tissue or relieve the underlying causes of kidney disease.
Understanding how nephron stem cells are maintained and characterised
The kidney is a tricky organ for regenerative treatment options. A kidney has millions of functional units called ‘nephrons’ which develop from kidney stem cells in utero.
Once a child is born, no further nephrons can be created within the kidney, regardless of any damage or disease that may impact their ability to function properly. In our laboratory, we have recently discovered a method of recreating these kidney stem cells, which has enabled us to create mini-kidney ‘organoids’.
We are continuing to learn how these stem cells can be best maintained in order to improve our development of kidney organoids for regenerative treatment options, drug screening and disease modelling applications.
Other projects
- Screening for novel treatments for congenital nephrotic syndrome
- Screening for novel treatments for Autosomal recessive
polycystic kidney disease ( ARPKD) - Tissue scale-up for transplantation
- Evaluation of connectivity and vascularisation at transplantation
- Integrating collecting duct tissue into kidney organoids
- Optimisation of nephron patterning and maturation
- Evaluation of the impact of macrophages on kidney morphogenesis
Funding
- Novo Nordisk Foundation
- Medical Research Future Fund Stem Cell Therapies Mission
- Medical Research Future Fund Genomic Health Futures Mission
- National Health & Medical Research Council of Australia
- PKD Australia and PKD USA
- Department of Jobs Precincts and Regions, Victorian State Government
- National Institutes of Health, USA
Collaborations
- Leiden University Medical Center, The Netherlands
- Prof. Anton J Rabelink
- University of Pennsylvania, USA
- Dr. Alexander Hughes
- Dr. Lukasz Bujacz
- The Royal Children’s Hospital, Melbourne
- Dr. Cathy Quinlan
- Dr. Thomas Forbes
- Dr. Sue White
Featured publications
Cellular extrusion bioprinting improves kidney organoid reproducibility and conformation. 2021.
+ Show/hide all publications
- Direct reprogramming to human nephron progenitor-like cells using inducible piggyBac transposon expression of SNAI2-EYA1-SIX1. 2019
- DNA Methyltransferase 1 Controls Nephron Progenitor Cell Renewal and Differentiation. 2019
- Evaluation of variability in human kidney organoids. 2019
- Generating Kidney from Stem Cells. 2019
- Introducing a Spectrum of Long-Range Genomic Deletions in Human Embryonic Stem Cells Using Type I CRISPR-Cas. 2019
- Kidney micro-organoids in suspension culture as a scalable source of human pluripotent stem cell-derived kidney cells. 2019
- Lin28 and let-7 regulate the timing of cessation of murine nephrogenesis. 2019
- Nephron progenitor commitment is a stochastic process influenced by cell migration. 2019
- Outcomes Following Treatment of Maternal Hypercalcemia Due to CYP24A1 Pathogenic Variants. 2019
- Overexpression of IL-11 promotes premalignant gastric epithelial hyperplasia in isolation from germline gp130-JAK-STAT driver mutations. 2019
- Reporter-based fate mapping in human kidney organoids confirms nephron lineage relationships and reveals synchronous nephron formation. 2019
- Single cell analysis of the developing mouse kidney provides deeper insight into marker gene expression and ligand-receptor crosstalk. 2019
- Single-cell analysis reveals congruence between kidney organoids and human fetal kidney. 2019
- Vascular bioengineering of scaffolds derived from human discarded transplant kidneys using human pluripotent stem cell-derived endothelium. 2019
2018
- 3D organoid-derived human glomeruli for personalised podocyte disease modelling and drug screening. 2018
- A Novel Approach to Single Cell RNA-Sequence Analysis Facilitates In Silico Gene Reporting of Human Pluripotent Stem Cell-Derived Retinal Cell Types. 2018
- Advances in predictive in vitro models of drug-induced nephrotoxicity. 2018
- Bayesian inference of agent-based models: a tool for studying kidney branching morphogenesis. 2018
- Branching morphogenesis in the developing kidney is not impacted by nephron formation or integration. 2018
- Choosing an easier path or following your passion. 2018
- Crim1 is required for maintenance of the ocular lens epithelium. 2018
- Development of the Human Fetal Kidney from Mid to Late Gestation in Male and Female Infants. 2018
- Functional Assessment of Patient-Derived Retinal Pigment Epithelial Cells Edited by CRISPR/Cas9. 2018
- Hamartin regulates cessation of mouse nephrogenesis independently of Mtor. 2018
- Haploinsufficiency for the Six2 gene increases nephron progenitor proliferation promoting branching and nephron number. 2018
- Identification of an Immortalised Human Airway Epithelial Cell Line with Dyskinetic Cilia. 2018
- Meeting report of the 2017 KidGen Renal Genetics Symposium. 2018
- Patient-iPSC-Derived Kidney Organoids Show Functional Validation of a Ciliopathic Renal Phenotype and Reveal Underlying Pathogenetic Mechanisms. 2018
- Pneumococcal haemolytic uraemic syndrome in the postvaccine era. 2018
- Prolonged prenatal hypoxia selectively disrupts collecting duct patterning and postnatal function in male mouse offspring. 2018
- Renal Subcapsular Transplantation of PSC-Derived Kidney Organoids Induces Neo-vasculogenesis and Significant Glomerular and Tubular Maturation In Vivo. 2018
- Reproducibility and staging of 3D human retinal organoids across multiple pluripotent stem cell lines. 2018
- Restricted cell cycle is essential for clonal evolution and therapeutic resistance of pre-leukemic stem cells. 2018
- Simultaneous reprogramming and gene editing of human fibroblasts. 2018
- Wnt11 directs nephron progenitor polarity and motile behaviour ultimately determining nephron endowment. 2018
2017
- (Re)Building a Kidney. 2017
- Clinical-Grade Isolated Human Kidney Perivascular Stromal Cells as an Organotypic Cell Source for Kidney Regenerative Medicine. 2017
- Does Renal Repair Recapitulate Kidney Development? 2017
- Long-term remission with eculizumab in atypical haemolytic uraemic syndrome. 2017
- Making a Kidney Organoid Using the Directed Differentiation of Human Pluripotent Stem Cells. 2017
- Massively parallel sequencing and targeted exomes in familial kidney disease can diagnose underlying genetic disorders. 2017
- Mutations in DZIP1L, which encodes a ciliary-transition-zone protein, cause autosomal recessive polycystic kidney disease. 2017
- Optimizing Outcomes in Pediatric Renal Transplantation Through the Australian Paired Kidney Exchange Program. 2017
- Prenatal hypoxia leads to hypertension, renal renin-angiotensin system activation and exacerbates salt-induced pathology in a sex-specific manner. 2017
- Self-organisation after embryonic kidney dissociation is driven via selective adhesion of ureteric epithelial cells. 2017
2016
- A Cas9 Variant for Efficient Generation of Indel-Free Knockin or Gene-Corrected Human Pluripotent Stem Cells. 2016
- A strategy for generating kidney organoids: Recapitulating the development in human pluripotent stem cells. 2016
- Analysed cap mesenchyme track data from live imaging of mouse kidney development. 2016
- Cap mesenchyme cell swarming during kidney development is influenced by attraction, repulsion, and adhesion to the ureteric tip. 2016
- Clinical-Grade Isolated Human Kidney Perivascular Stromal Cells as an Organotypic Cell Source for Kidney Regenerative Medicine. 2016
- Crim1 has cell-autonomous and paracrine roles during embryonic heart development. 2016
- Cystatin C Based Equation Accurately Estimates Glomerular Filtration Rate in Children With Solid and Central Nervous System Tumours: Enough Evidence to Change Practice? 2016
- GAPTrap: A Simple Expression System for Pluripotent Stem Cells and Their Derivatives. 2016
- Generating kidney tissue from pluripotent stem cells. 2016
- Generation of kidney organoids from human pluripotent stem cells. 2016
- Neonatal vascularization and oxygen tension regulate appropriate perinatal renal medulla/papilla maturation. 2016
- Understanding kidney morphogenesis to guide renal tissue regeneration. 2016
2015
- A protocol for the identification and validation of novel genetic causes of kidney disease. 2015
- A spatially-averaged mathematical model of kidney branching morphogenesis. 2015
- Direct transcriptional reprogramming to nephron progenitors. 2015
- Generating a self-organizing kidney from pluripotent cells. 2015
- Improving our resolution of kidney morphogenesis across time and space. 2015
- Kidney organoids from human iPS cells contain multiple lineages and model human nephrogenesis. 2015
- Paediatric nephrology: the last 50 years. 2015
- Renal developmental defects resulting from in utero hypoxia are associated with suppression of ureteric ß-catenin signalling. 2015
- ROBO2 restricts the nephrogenic field and regulates Wolffian duct-nephrogenic cord separation. 2015
- Simultaneous Reprogramming and Gene Correction of Patient Fibroblasts. 2015
- The origin of the mammalian kidney: implications for recreating the kidney in vitro. 2015
1980s
- Xenogeneic antibodies with apparent public idiotypic specificity for anti-Ia.7 antibodies are directed in part against V kappa 21D and E subgroup marker. 1986
