Human immune cells produced in a dish in world first
A Melbourne research team has reproduced and visualised the earliest developmental steps in human immune cell production in the laboratory and are now set to advance our understanding of childhood diseases like leukemia and autoimmune conditions.
One day the advance could lead to a patient's own skin cells being used to produce new cells for cancer immunotherapy or to test autoimmune disease interventions.
The group, led by Professors Ed Stanley and Andrew Elefanty, from the Murdoch Children's Research Institute in Melbourne, Australia, said the work has added definitive evidence about how the body's earliest immune cells are formed.
These lymphocytes are produced by cells which form the embryo's first organs rather than the blood-producing stem cells that sit inside the body's bone marrow.
The research combined two powerful laboratory techniques, genetic engineering and a novel way of growing stem cells, to make the breakthrough, which has been published in the prestigious journal Nature Cell Biology.
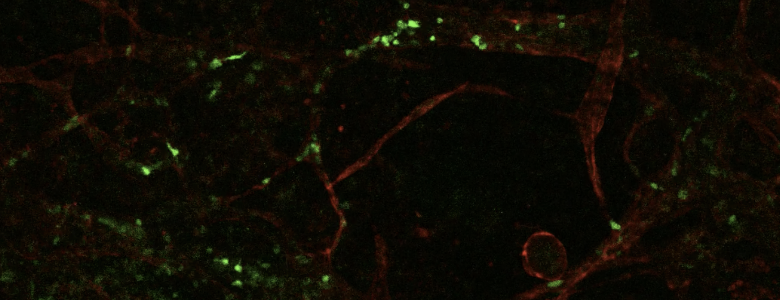
First, the team engineered pluripotent stem cells to glow green when a specific protein marker of early immune cells, RAG1, was switched on. RAG1 is responsible for creating the immune response to infections and vaccines.
Next, the team isolated the glowing green RAG1-positive cells and showed that they could also form multiple immune cell types, including cells required for shaping the development of the whole immune system.
"We think these early cells might be important for the correct maturation of the thymus, the organ that acts as a nursery for T-cells" said Professor Stanley.
"These RAG1 cells are like the painters and decorators who set up that nursery, making it a safe and cosy environment for later-born immune cells," he said.
Professor Elefanty said, "Although a clinical application is likely still years away, we can use this new knowledge to test ideas about how diseases like childhood leukemia and type 1 diabetes develop. Understanding more about the steps these cells go through, and how we can more efficiently nudge them down a desired pathway, is going to be crucial to that process."
The study was funded by the National Health and Medical Research Council*, the Australian Research Council, the Children's Cancer Research Foundation (Australia) and the Stafford Fox Medical Research Foundation, and involved researchers from the University of Melbourne, Monash University and the Walter and Eliza Hall Institute.
Publication: Multipotent RAG1+ progenitors emerge directly from haemogenic endothelium in human pluripotent stem cell-derived haematopoietic organoids. Nature Cell Biology January 2019
DOI: 10.1038/s41556-019-0445-8
Available for interview:
Professor Ed Stanley
Professor Andrew Elefanty
Media Contact:
Bridie Byrne
MCRI communications specialist
+61 403 664 416
show email address



