Concussion Research
Understanding concussion recovery in young people
Our research goals
- Transform concussion treatment: We focus on redefining treatment for children and adolescents by identifying the most effective methods to accelerate and support recovery.
- Recovery insights: Our research aims to deepen the understanding of how young people recover from concussions.
- Biomarker identification: We seek to identify biomarkers, such as brain imaging and blood proteins, and risk factors that contribute to prolonged concussion recovery.
- Enhanced access to evidence-based management: We seek to improve access for parents and communities to evidence-based concussion management strategies.
More information
- Concussion Essentials (HeadCheck) app: Access our comprehensive app for concussion management.
- Concussion Podcasts: Listen to our latest podcasts on concussion research and recovery.
- A-Z Concussion: Explore our detailed A-Z guide on concussion.
Contact us
Get in contact with the Concussion Research team.
Email:
show email address
Group Leaders

Our projects
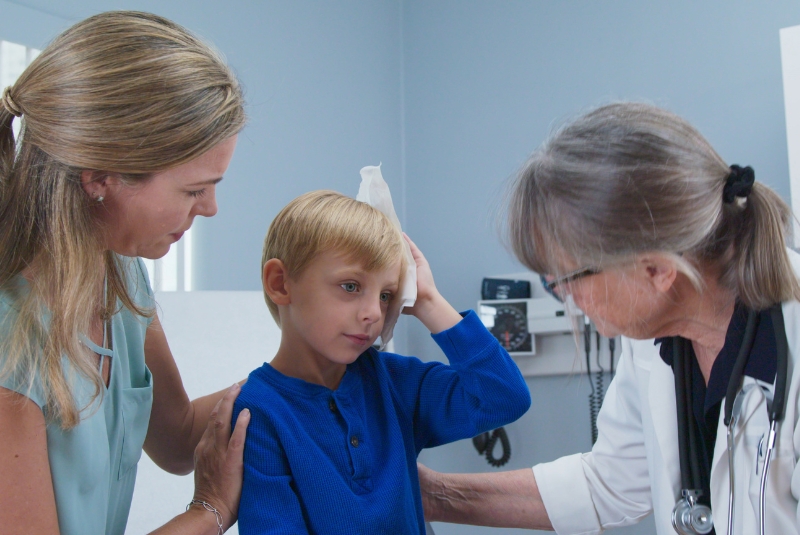
Concussion Essentials Clinic implementation project
This clinical trial evaluates the implementation of concussion interventions within a new paediatric clinical service, the MCRI Concussion Clinic, and assesses clinical outcomes for children and adolescents.
Currently, concussion care in Victoria is fragmented. Families must navigate a complex system and find providers with varying levels of expertise. There is no centralised, evidence-based paediatric concussion clinic available, this trial aims to change that.
Read more...
Mental Health following mild Traumatic Brain Injury in Adolescent
This study investigates mental health outcomes and associated factors, such as family environment, social participation, and quality of life, in adolescents following mild traumatic brain injury (mTBI).
Read more...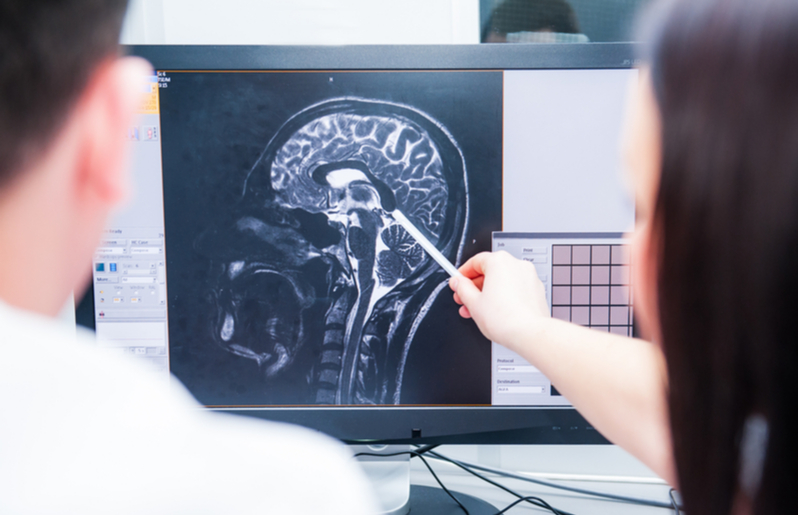
Traumatic Brain Injury Research
Investigating the mental health outcomes in adolescents with mild traumatic brain injury. There are many causes of brain injury, including traffic accidents, sports accidents or lack of oxygen to the brain. This project helps you find out about Acquired Brain Injury (ABI) research that is currently happening on the Melbourne Children's Campus.
Read more...Concussion Essentials (HeadCheck) app
An evidence-based smartphone application, developed in collaboration with the AFL and Curve Tomorrow. Designed using the latest scientific knowledge of concussion, the app provides ready access to current clinical best practices regarding adult and paediatric concussion.
The app includes a sideline assessment tool and provides individually tailored guidance to help users or parents manage a safe return to normal activities (school, study, work, exercise, and sport).
Rehabilitation of Executive Function in Paediatric Traumatic Brain Injury (REPEAT Study)
This study investigated the impact of computer activities and their effectiveness in improving memory and making decisions in children with post-traumatic brain injury (TBI). TBI refers to any damage to the brain acquired as a result of a trauma, such as injuries caused by external forces such as falls, contact sports, and accidents.
Training Attention after Brain Injury in Children
We are interested in understanding whether a game-based attention training program can strengthen attention in children who have experienced an acquired brain injury (ABI). This is a collaboration between The Monash School of Psychological Sciences and the Murdoch Children's Research Institute.
Take CARe Biomarkers
Followed children and adolescents for up to three months post-concussion, examining symptoms, MRI brain imaging, blood biomarkers, cognition (thinking abilities), physical function, parent and child mental health, quality of life, and cost of concussion.
Funding
Thank you to our supporters.
- The Royal Children’s Hospital Foundation
- National Health and Medical Research Council (NHMRC)
- Medical Research Future Fund (MRFF)
Featured publications
Gornall, Alice & Takagi, Michael & Morawakage, Thilanka & Liu, Xiaomin & Anderson, Vicki. (2021). Mental health after paediatric concussion: a systematic review and meta-analysis. British Journal of Sports Medicine. 55. bjsports-2020. 10.1136/bjsports-2020-103548.
Shapiro JS, Takagi M, Silk T, Anderson N, Clarke C, Davis GA, Hearps SJC, Ignjatovic V, Rausa V, Seal ML, Babl FE, Anderson V. No Evidence of a Difference in Susceptibility-Weighted Imaging Lesion Burden or Functional Network Connectivity between Children with Typical and Delayed Recovery Two Weeks Post-Concussion. J Neurotrauma. 2021 Sep 1;38(17):2384-2390. doi: 10.1089/neu.2021.0069. Epub 2021 Jul 30. PMID: 33823646; PMCID: PMC8881952.
Shapiro JS, Hearps S, Rausa VC, Anderson V, Anderson N, Pugh R, Chau T, Clarke C, Davis GA, Fabiano F, Fan F, Parkin GM, Takagi M, Babl FE. Validation of the SCAT5 and Child SCAT5 Word-List Memory Task. J Neurotrauma. 2022 Jan;39(1-2):138-143. doi: 10.1089/neu.2020.7414. Epub 2021 May 10. PMID: 33765839.
Anderson V, Rausa VC, Anderson N, Parkin G, Clarke C, Davies K, McKinlay A, Crichton A, Davis GA, Dalziel K, Dunne K, Barnett P, Hearps SJ, Takagi M, Babl FE. Protocol for a randomised clinical trial of multimodal postconcussion symptom treatment and recovery: the Concussion Essentials study. BMJ Open. 2021 Feb 11;11(2):e041458. doi: 10.1136/bmjopen-2020-041458. PMID: 33574145; PMCID: PMC7880104.
Rausa VC, Shapiro J, Seal ML, Davis GA, Anderson V, Babl FE, Veal R, Parkin G, Ryan NP, Takagi M. Neuroimaging in paediatric mild traumatic brain injury: a systematic review. Neurosci Biobehav Rev. 2020 Nov;118:643-653. doi: 10.1016/j.neubiorev.2020.08.017. Epub 2020 Sep 6. PMID: 32905817.
+ Show/hide all publications
2020
- Clarke et al., (2020). Child concussion recognition and recovery: a community delivered, evidenced-based solution. Annals of Translational Medicine.
- Bressan et al., (2020). Use of the sport concussion assessment tools in the emergency department to predict persistent post-concussive symptoms in children. Journal of Paediatrics and Child Health.
- Shapiro et al., (2020). Examining Microstructural White Matter Differences between Children with Typical and Those with Delayed Recovery Two Weeks Post-Concussion. Journal of Neurotrauma
- Teh et al., (2020). Acute cognitive postconcussive symptoms follow longer recovery trajectories than somatic postconcussive symptoms in young children. Brain Injury.
- Anderson et al., (2020). Trajectories and Predictors of Clinician-Determined Recovery after Child Concussion. Journal of Neurotrauma.
- Truss et al., (2020). Trajectories and Risk Factors for Pediatric Postconcussive Symptom Recovery.
2019
- Takagi et al., (2019). Does a computerized neuropsychological test predict prolonged recovery in concussed children presenting to the ED? Child Neuropsychology.
- Takagi et al., (2019). Protocol for a prospective, longitudinal, cohort study of recovery pathways, acute biomarkers, and cost for children with persistent post-concussion symptoms: the Take CARe Biomarkers study. BMJ Open.
- Parkin et al., (2019). Plasma TNF alpha is a predictor of persisting symptoms post-concussion in children. Journal of Neurotrauma.
- Gornall et al., (2019). Behavioral and emotional difficulties following pediatric concussion. Journal of Neurotrauma.
2018 - 2016
- Rausa et al., (2018). Predicting concussion recovery in children and adolescents in the emergency room. Current Neurology and Neuroscience Reports.
- Lugones et al., (2018). Blood biomarkers in paediatric mild traumatic brain injury: a systematic review. Neuroscience and Behavioural Reviews.
- Truss et al., (2017). Trajectories and Risk Factors for Posttraumatic Stress Symptoms Following Pediatric Concussion. Journal of Neurotrauma.
- Davis G et al., (2017). What is the difference in concussion management in children as compared to adults? A systematic review. British Journal of Sports Medicine.
- Hearps et al., (2017). Validation of a score to determine time to post-concussive recovery. Pediatrics,
- Bressan et al., (2016). Protocol for a prospective, longitudinal, cohort study of post-concussive symptoms in children: the Take C.A.Re (Concussion Assessment and Recovery Research) study. BMJ Open.
